Visceral artery aneurysms – classification, diagnosis and treatment
 Affiliation and address for correspondence
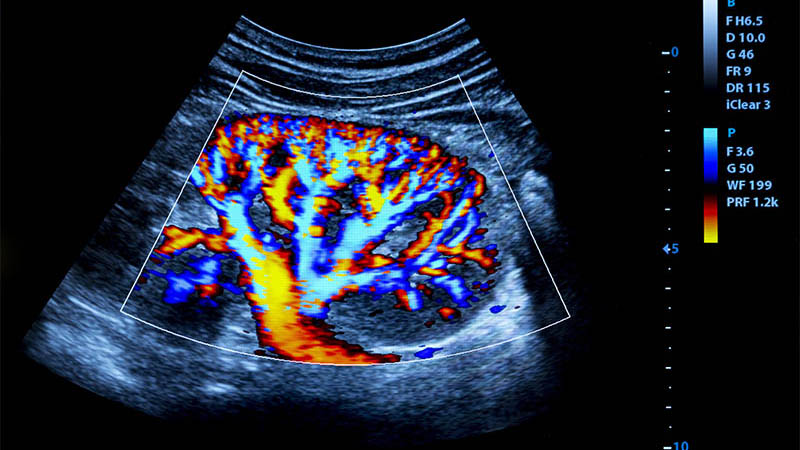
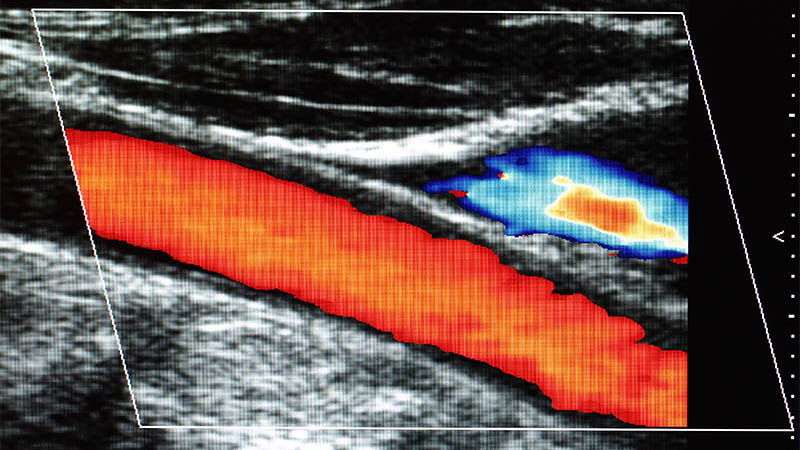
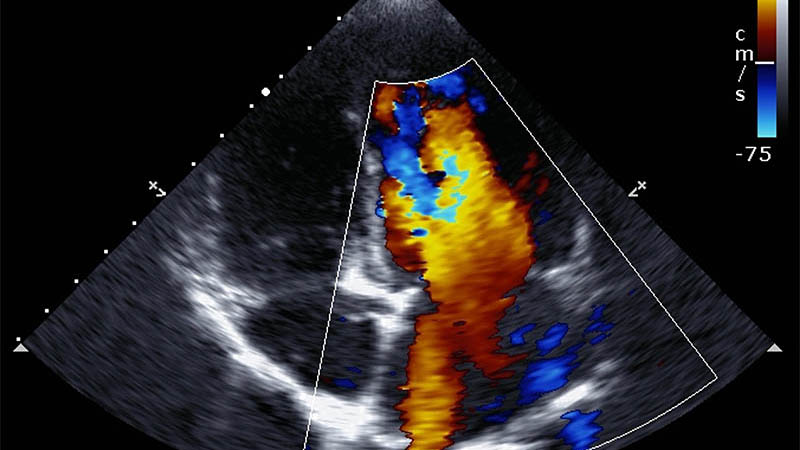
Affiliation and address for correspondenceAlthough visceral artery aneurysms are rare, mortality due to their rupture is high, estimated at even 25–75%. That is why it is significant to detect each such lesion. Visceral artery aneurysms are usually asymptomatic and found incidentally during examinations performed for other indications. Autopsy results suggest that most asymptomatic aneurysms remain undiagnosed during lifetime. Their prevalence in the population is therefore higher. The manifestation of a ruptured aneurysm depends on its location and may involve intraperitoneal hemorrhage, gastrointestinal and portal system bleeding with concomitant portal hypertension and bleeding from esophageal varices. Wide access to diagnostic tests, for example ultrasound, computed tomography or magnetic resonance imaging, helps establish the correct diagnosis and a therapeutic plan as well as select appropriate treatment. After a procedure, the same diagnostic tools enable assessment of treatment efficacy, or are used for the monitoring of aneurysm size and detection of potential complications in cases that are ineligible for treatment. The type of treatment depends on the size of an aneurysm, the course of the disease, risk of rupture and risk associated with surgery or endovascular procedure. Endovascular treatment is preferred in most cases. Aneurysms are excluded from the circulation using embolization coils, ethylene vinyl alcohol, stents, multilayer stents, stent grafts and histoacryl glue (or a combination of these methods).