Diabetic foot syndrome: Charcot arthropathy or osteomyelitis? Part I: Clinical picture and radiography
Aleksandra Konarzewska1, Anna Korzon-Burakowska2, Ludomira Rzepecka-Wejs3, Iwona Sudoł-Szopińska4, Edyta Szurowska1, Michał Studniarek5
 Affiliation and address for correspondence
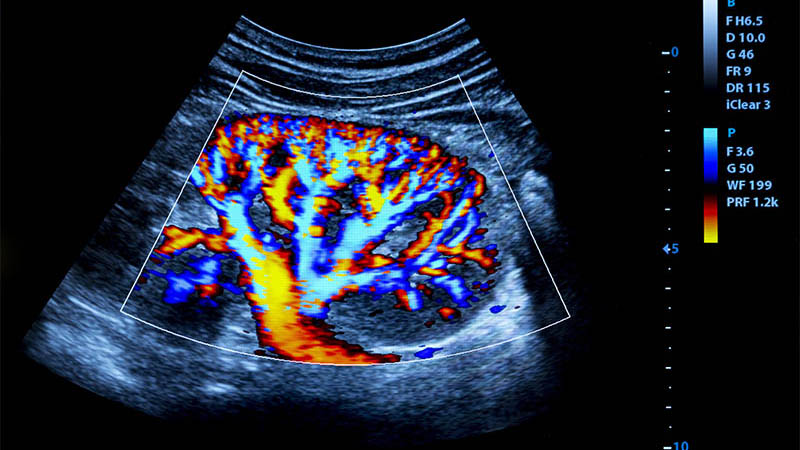
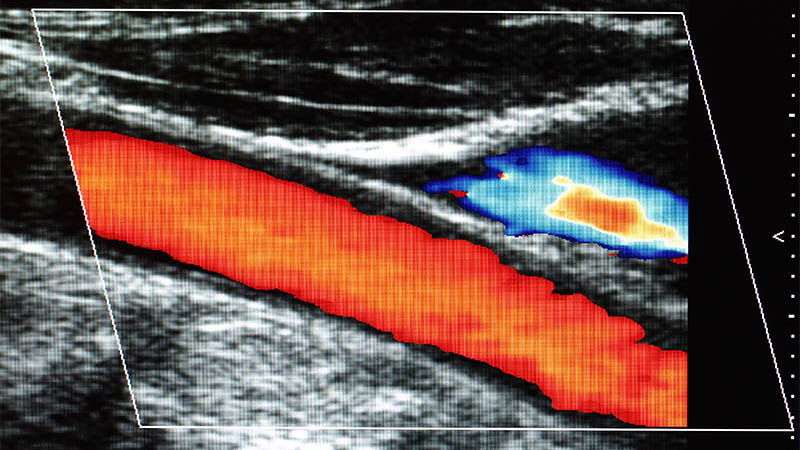
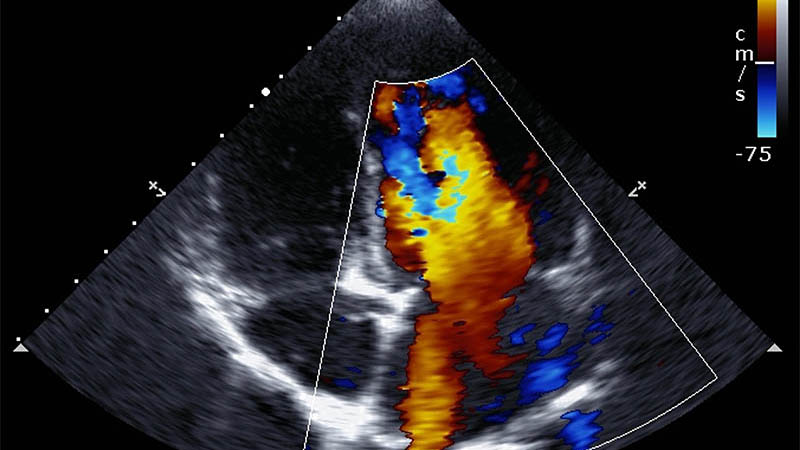
Affiliation and address for correspondenceOne of significant challenges faced by diabetologists, surgeons and orthopedists who care for patients with diabetic foot syndrome is early diagnosis and differentiation of bone structure abnormalities typical of these patients, i.e. osteitis and Charcot arthropathy. In addition to clinical examination, the patient’s medical history and laboratory tests, imaging plays a significant role. The evaluation usually begins with conventional radiographs. In the case of osteomyelitis, radiography shows osteopenia, lytic lesions, cortical destruction, periosteal reactions as well as, in the chronic phase, osteosclerosis and sequestra. Neurogenic arthropathy, however, presents an image resembling rapidly progressing osteoarthritis combined with aseptic necrosis or inflammation. The image includes: bone destruction with subluxations and dislocations as well as pathological fractures that lead to the presence of bone debris, osteopenia and, in the later phase, osteosclerosis, joint space narrowing, periosteal reactions, grotesque osteophytes and bone ankylosis. In the case of an unfavorable course of the disease and improper or delayed treatment, progression of these changes may lead to significant foot deformity that might resemble a “bag of bones”. Unfortunately, radiography is non-specific and frequently does not warrant an unambiguous diagnosis, particularly in the initial phase preceding bone destruction. For these reasons, alternative imaging methods, such as magnetic resonance tomography, scintigraphy, computed tomography and ultrasonography, are also indicated.